By Dr. David Gorstein, Partner & Population Health Practice Leader
Recent analyses put the “longevity market” at over $1T in total addressable value. That opportunity is typically framed around demand for:
- $10K–$50K “longevity retreats”
- Extensive multi-omic panels
- Stacks of peptides and nootropics
- Unvalidated “biological age” tests used for serial monitoring
- Concierge “longevity” clinics that over-test and over-image as a business model
This is a compelling story for investors. It is far less compelling if the goal is to extend healthspan in a way that would meet even minimal value-based care standards.
The uncomfortable truth is that the core pillars of healthspan are already well studied, actionable, and essentially free.
- Regular physical activity (at least 150–300 minutes per week of moderate intensity, plus at least 2 days per week of strength training)
- Sleep regularity and sufficiency
- Tobacco cessation and minimal alcohol
- Vaccination, blood pressure and lipid control, and basic metabolic risk management
- Social connection, fall prevention, and fracture prevention in older adults
These “boring” levers are exactly the ones that move mortality curves, disability curves, and dementia curves the most. They are not scarce, and they are not high-margin.
If your goals are like mine:
- Can I ride a bike at 70?
- Can I climb stairs without stopping?
- Am I still myself cognitively?
- Can I chase my grandchildren without worrying about my balance?
then most of the tools you need already sit in primary care, public health, and your own behavior, not in a boutique longevity stack.
A Different Map: Evidence vs. Scalability
Instead of organizing the longevity market by price point or “innovation,” it is more useful to classify interventions along two axes:
Evidence: strength of data for improving meaningful outcomes (mortality, morbidity, function, quality of life)
Scalability: feasibility to deploy at population scale at acceptable cost and risk
This yields four quadrants.
- High-Value, Population-Level
Definition: Strong evidence; cheap; scalable; low harm.
Examples:
- Physical activity prescriptions with resistance training
- Sleep regularity and duration programs
- Tobacco cessation and alcohol reduction
- Vaccination; blood pressure and lipid control; simple metabolic risk management
- Social connection initiatives; fall and fracture prevention
These are the true “blockbusters” of healthspan. They are exactly what a rational value-based system would buy first, at scale.
They are always mentioned in longevity marketing, but then the pitch quickly pivots to the shiny new objects with little or no evidence to support them.
- High-Value, Targeted / High-Risk
Definition: Strong evidence in clearly defined, higher-risk populations; often pharmacologic or procedure-based.
Examples:
- SGLT2 inhibitors and GLP-1 agonists for established cardiometabolic disease or obesity
- Antihypertensives and statins in high-risk groups
- Proven secondary-prevention interventions (post-MI, stroke, high-risk heart failure, osteoporosis with prior fragility fracture)
These belong in a longevity conversation, but as precision tools, not wellness accessories.
- Low-Value, Scalable
Definition: Easy to sell and scale; weak or indirect evidence for hard outcomes; often marketed via biomarkers and engagement metrics instead of morbidity and mortality.
Illustrative examples:
- Serial, unvalidated “biologic age” tests treated as primary endpoints
- Consumer multi-omic panels with no clear treatment pathways
- General-population continuous monitoring with no structured, evidence-based intervention behind the data
These offerings may generate insight, motivation, or a sense of control for some individuals. As core longevity infrastructure, however, they have a poor evidence-to-cost ratio and are easy vehicles for over-claiming.
- High-Uncertainty / Experimental
Definition: Biologically plausible and often exciting, but with limited or early evidence for clinically meaningful endpoints.
Illustrative examples:
- Many peptides, stacks of nootropics, and “longevity cocktails”
- Intensive multi-omic plus imaging packages in otherwise healthy people
- High-priced longevity retreats and concierge clinics that bundle speculative interventions with a clinical veneer
These are not inherently illegitimate. They are research questions or luxury goods, not standard of care. The problem arises when they are sold and reimbursed as if they occupy the high-value, population-level quadrant.
Exhibit: The Longevity Intervention Matrix
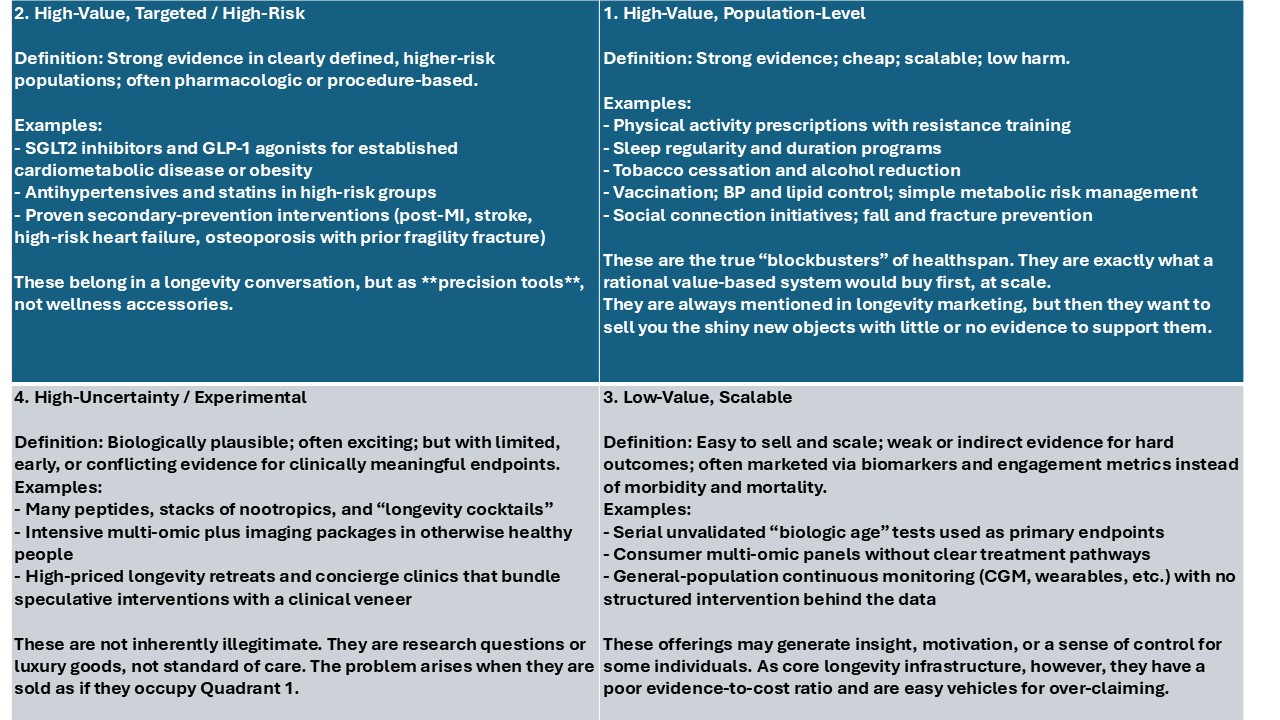
Axes:
Vertical: Evidence for meaningful outcomes
Horizontal: Scalability at acceptable cost and risk
HIGH VALUE longevity interventions are the upper right quadrant
The key takeaway for systems, payers, and employers is simple:
- Start in the high-value, population-level quadrant as the default; these give the highest health return per dollar.
- Use the targeted, high-risk quadrant selectively, for clearly defined groups, with outcome and cost accountability.
- Treat the low-value, scalable quadrant at best as an engagement layer, not core healthspan infrastructure.
- Treat the experimental quadrant explicitly as research or luxury, not standard care
Recommendations for Systems, Payers, and Employers
To align “longevity” with genuine value-based care, stakeholders should:
- Reallocate investment
Prioritize infrastructure and programs that increase movement, strength, sleep regularity, cardiometabolic control, and fall prevention across the population.
Fund digital and in-person interventions that scale these basics, not boutique offerings.
- Risk-stratify higher-cost interventions
Reserve advanced pharmacology, imaging, and intensive monitoring for clearly defined high-risk cohorts, with accountability for total cost and net benefit, not just service volume.
- Reframe boutique longevity as research or luxury, not standard care
Encourage transparent labeling of speculative or high-priced interventions as experimental or elective.
Avoid embedding them in benefit designs as if they were evidence-based essentials.
- Measure what matters
Track outcomes that people actually care about and understand: mobility, independence, cognitive function, hospitalizations, and days at home, alongside mortality.
Evaluate any “longevity program” against those outcomes and total cost, not against proprietary biomarkers alone.
- Define success in human terms
Anchor programs on the outcomes people actually care about in later life: mobility, cognition, independence, and the ability to participate in relationships and roles—not just nicer dashboards.
Conclusion
“Longevity” is a useful public-facing language only if it ultimately describes more healthy, independent years for more people per dollar, not just a new total addressable market for the wellness and biotech industries.
High-value longevity care already exists, and it looks far more like safe sidewalks, resistance training, blood pressure control, vaccination, and boring sleep routines than it does like $25,000 retreats or multi-omic dashboards. The task now is to fund and scale the former while being honest about the latter.
